
Title: Depressive and Bipolar Disorders Crash Course Psychology 30
Channel: CrashCourse
Depressive and Bipolar Disorders Crash Course Psychology 30 by CrashCourse
clinical depression bipolar disorder, major depression bipolar disorder, severe depression bipolar disorder, major bipolar depression disorder symptoms, clinical depression vs bipolar disorder, major depression and bipolar disorder are quizlet, major depression with bipolar disorder icd 10, major depression and bipolar disorders are most characteristic of which of the following, major depression and bipolar disorder similarities, what do clinical depression and bipolar disorder have in common
Is Your Depression Actually Bipolar? The Shocking Truth You NEED to Know
Battling the Blues? Could It Be More Than Just Depression?
It's easy to feel lost when struggling with persistent sadness. You might think you understand the source of your emotional turmoil. But, what if there’s a twist? What if those low feelings aren't just garden-variety depression? What if something else is at play? Let's explore a possibility that many people overlook: bipolar disorder.
The Elusive Nature of Mood Swings: Unraveling the Mystery
Depression is a complex beast. It can manifest in many ways. For some, it's a constant weight. It's a feeling of hopelessness that clings persistently. Others might experience bouts of intense sadness. It can be difficult to climb out of the darkness. It's important to remember that not all feelings of sadness are the same. However, the narrative changes when mood swings enter the picture. If you've experienced highs and lows, it might indicate something different.
Beyond the Blues: Recognizing the Signs of Bipolar Disorder
Bipolar disorder involves significant shifts in mood. These shifts can vary. They range from manic episodes to depressive episodes. During manic episodes, people feel euphoric. They can also have an increase in energy. They may experience racing thoughts. Some engage in impulsive behaviors. These behaviors can include reckless spending. They can also involve making risky decisions. Conversely, depressive episodes mirror the symptoms of major depression. These symptoms include persistent sadness and loss of interest. Additionally, there may be fatigue or changes in appetite. You probably wonder, where's the truth?
Manic Episodes: A Glimpse into the Upside Down
The manic phase can be as confusing as the depressive one. People may feel on top of the world. They often experience an inflated sense of self-esteem. They might suddenly have grand ideas. They may take on many projects at once. Speech may become rapid and pressured. Sleep can be reduced. It's important to note that these behaviors are not always easy to identify. Friends and family members may notice changes. They might observe uncharacteristic behavior. These behaviors can be concerning.
Depressive Episodes: The Weight of the World
Depressive episodes are often easier to recognize. They share many symptoms with regular depression. Individuals may feel overwhelmingly sad. They often lose interest in activities. They may withdraw from social situations. Fatigue and changes in sleep patterns are common. Feelings of hopelessness and worthlessness can be unbearable. It's a significant part of the bipolar condition.
The Overlap: Depression and Bipolar Disorder's Shared Territory
It's easy to see how things can become blurry. Both depression and bipolar depression share similarities. It's a reason why misdiagnosis is surprisingly common. Both present sadness. Both feature low energy. It's crucial to differentiate between them for effective treatment. But, how? The presence of manic or hypomanic episodes is the key.
Seeking Help: Understanding Your Options
If you suspect you may have bipolar disorder, seek professional help. A doctor or mental health expert can help. They can assess your symptoms. They will also evaluate your history. This will allow them to make an accurate diagnosis. Therapies, such as cognitive behavioral therapy (CBT), are available. They can teach coping strategies. Medication may also be crucial. It can help regulate mood swings. There's always hope.
The Importance of Accurate Diagnosis: A Path to Well-being
Getting the right diagnosis is critical. It is the initial step towards recovering. It allows for appropriate treatment. It is the foundation for your mental wellness. With it, you can get your life back. Incorrect diagnoses can lead to ineffective treatment. This delays improving your mental health. A correct diagnosis is empowering. It acknowledges your struggle. It also opens doors to a fulfilling life.
Living with Bipolar Disorder: Managing the Journey
Life with bipolar disorder requires ongoing management. Consistency in medication and therapy is vital. You should learn to recognize triggers. You should also develop coping mechanisms. Building a strong support system is key. Support can come from friends, family, or support groups. It’s a continuous process. However, it's definitely manageable. You can live a meaningful life.
A Note of Encouragement: You Are Not Alone
Dealing with mood disorders can be very isolating. Recognize that you aren't alone. Many people experience similar struggles. Support is readily available. You can find it. You can improve your mental well-being. Take the first steps towards getting help. Embrace the journey. This is your life. Make it count!
Vanderbilt Depression Screening: Is THIS the Silent Killer Stealing YOUR Happiness?Is Your Depression Actually Bipolar? The Shocking Truth You NEED to Know
Hey everyone, let’s talk about something really important: mental health. Specifically, let's delve into the complexities of depression and the possibility that it's not just depression you're experiencing. It might be something else entirely, something often misunderstood and sometimes overlooked: bipolar disorder. I know, it sounds a bit dramatic, but trust me, we need to understand this. Many people are struggling, and knowing the difference – and getting the right help – can be life-changing. Think of it as navigating a tricky map, where the wrong path leads to a frustrating dead end, but the correct one leads to real recovery and a better quality of life. We’re going to unpack this together.
1. The Shadow of Depression: More Than Meets the Eye
Depression. We've all likely felt its heavy cloak at some point, haven't we? The persistent sadness, the lack of energy, the feeling of being completely overwhelmed. It's like wading through treacle, every step a struggle. But what if that "treacle" isn't always just depression? What if it's a symptom of something deeper, more dynamic, something that swings like a pendulum? That’s where bipolar disorder comes into the picture. It's a condition characterized by extreme shifts in mood, from periods of intense sadness and hopelessness (the depressive episodes) to periods of elevated mood, energy, and impulsivity (the manic or hypomanic episodes). We're talking about a rollercoaster, not just a slow descent.
2. Decoding the Depths: What Exactly Is Bipolar Disorder?
Bipolar disorder is a mental health condition that causes extreme shifts in mood, energy levels, and activity levels. Think of it like a seesaw, constantly going up and down. There are different types of bipolar disorder, and the severity and nature of the episodes can vary widely from person to person. Some people experience full-blown manic episodes, which can involve risky behaviors, racing thoughts, and a feeling of invincibility. Others experience hypomanic episodes, which are less severe but still involve elevated mood and energy. The key is understanding that these mood swings aren't just "moody days" – they're disruptive and significantly impact daily life. This is not something you can "snap out of".
3. The Misdiagnosis Maze: Why Depression Sometimes Masks Bipolar
Here’s where it gets tricky. Depression is often the initial presenting symptom, the thing that gets someone to seek help. It's the visible iceberg tip. Clinicians, understandably, often start with a diagnosis of major depressive disorder. The problem? If the underlying cause is bipolar disorder, treating only the depression without addressing the mood swings can be like putting a bandage on a gaping wound. Antidepressants, while helpful for depression, can sometimes trigger or worsen manic episodes in people with bipolar disorder, making the situation even more unstable.
4. Unmasking the Manic Side: Recognizing the Upward Swing
So, how do you spot the manic or hypomanic episodes? This is crucial. These episodes are characterized by:
- Elevated mood: Feeling unusually happy, euphoric, or irritable.
- Increased energy and activity: Feeling restless, talking a mile a minute, and having lots of new ideas.
- Racing thoughts: A feeling of your thoughts jumping from one thing to another.
- Decreased need for sleep: Feeling wide awake even after minimal sleep.
- Impulsive behavior: Spending sprees, reckless driving, substance abuse, or other risky behaviors.
- Inflated self-esteem: Feeling unusually confident or believing you have special powers.
It can be like a supernova bursting within you, a blinding light of energy and exuberance; it's captivating, but also destructive.
5. The Hypomanic High: A Subtle Shift?
Hypomania is a milder form of mania. It can feel incredibly productive and creative. You might feel like you're on top of the world, with boundless energy and a flood of brilliant ideas. But the key is recognizing the difference between productive, energized behavior and hypomania. Sometimes, it can seem perfectly normal, but it has the potential to evolve to a more severe state. It requires careful observation and, ideally, tracking.
6. The Depressive Doldrums: Recognizing the Downward Spiral
The depressive episodes associated with bipolar disorder are often indistinguishable from those of major depressive disorder. The symptoms include:
- Persistent sadness, hopelessness, or emptiness.
- Loss of interest in activities you once enjoyed.
- Changes in appetite or weight.
- Sleep disturbances (insomnia or oversleeping).
- Fatigue or loss of energy.
- Difficulty concentrating or making decisions.
- Feelings of worthlessness or guilt.
- Thoughts of death or suicide.
It's like being trapped in a dark room, with no light and no escape.
7. The Diagnostic Dance: How Professionals Tell the Difference
Diagnosing bipolar disorder can be complex. There isn’t a single lab test. Professionals, be they psychiatrists or psychologists, rely on a combination of:
- Thorough medical history: Discussing your symptoms, family history of mental illness, and any past treatments.
- Symptom tracking: Keeping a journal to track your mood, sleep patterns, and behaviors.
- Psychological evaluation: Assessing your overall mental state, including your thoughts, feelings, and behaviors.
- Observation: Observing patterns of behavior and reactions during therapy.
It's a process, a detective uncovering clues to solve the mystery of your mental health.
8. Family Matters: The Genetic Link to Bipolar Disorder
Bipolar disorder often runs in families. If a close relative has the condition, your risk increases. This doesn't mean you'll automatically develop it, but it does suggest a genetic predisposition. Think of it like a family heirloom; it might be passed down from generation to generation, and you need to know how to handle it or the consequences it introduces.
9. Beyond Medication: The Power of Therapy and Lifestyle Changes
Medication, usually mood stabilizers and sometimes antidepressants (with careful monitoring), is often the cornerstone of treatment for bipolar disorder. But it’s not the only tool in the toolbox. Therapy, such as cognitive-behavioral therapy (CBT) and interpersonal and social rhythm therapy (IPSRT), can help you manage your moods, develop coping skills, and establish healthy routines. Lifestyle changes, such as regular sleep, a healthy diet, and exercise, are also critical.
10. The Stigma Game: Breaking the Silence
One of the biggest obstacles to getting help is stigma. Mental illness, including bipolar disorder, still carries a stigma that can prevent people from seeking the treatment they need. We need to talk about it openly and honestly, and create a supportive environment where people feel comfortable seeking help without judgment. It's crucial to remember you're not alone and there is no shame in seeking help.
11. The Importance of Early Intervention: Time is of the Essence
The earlier bipolar disorder is diagnosed and treated, the better the long-term outcome. Early intervention can help prevent the condition from worsening and minimize the impact on your life. So, if you suspect you or someone you know might have bipolar disorder, don't delay seeking professional help. It's like preventing a wildfire: faster response; less damage.
12. Living Victoriously: Managing Bipolar Disorder Long-Term
Living with bipolar disorder requires ongoing management. This includes:
- Taking medication as prescribed.
- Attending therapy sessions regularly.
- Monitoring your mood and recognizing early warning signs.
- Establishing and sticking to a regular routine.
- Avoiding drugs and alcohol.
- Building a strong support system.
It's a marathon, not a sprint.
13. Building a Supportive Network: Your Circle of Strength
Having a strong support system is crucial. This may include family, friends, therapists, support groups, and other healthcare professionals. Sharing your experiences and feelings with others who understand can make all the difference. It's never a solo journey. Lean on those who care for you.
14. Staying Informed: The Ongoing Pursuit of Knowledge
The field of mental health is constantly evolving. Staying informed about the latest research and treatment options is essential. Read books, articles, and websites, and talk to your healthcare provider about any new developments. Knowledge is power, and it empowers you to take an active role in your health.
15. A Path to Understanding: Your Journey to a Better Life
Understanding that your "depression" might actually be bipolar disorder is a crucial first step. It's like finding the correct key to unlock a door to treatment and recovery. Remember, you're not alone. Millions of people live fulfilling lives with bipolar disorder. With the right treatment, support, and self-awareness, you can too. This is a challenge, yes, but it's also a chance to build a life of resilience, understanding, and joy.
Closing Thoughts
Navigating mental health can feel like scaling Mount Everest, but having the correct gear and a reliable guide can make all the difference. Knowing the difference between depression and bipolar disorder is essential, as the correct diagnosis can lead to the right treatment. Don't hesitate to reach out for help if you're struggling. Your mental health is important!
FAQs: Your Questions, Answered
- **How do
Bipolar Disorder Symptoms, Risk Factors, Causes, Diagnosis and Treatments, Animation
By Alila Medical Media Bipolar Disorder Symptoms, Risk Factors, Causes, Diagnosis and Treatments, Animation by Alila Medical Media
Bipolar and related disorders - causes, symptoms, treatment & pathology Updated 2024

By Osmosis from Elsevier Bipolar and related disorders - causes, symptoms, treatment & pathology Updated 2024 by Osmosis from Elsevier

Title: Daily Routine for Bipolar Disorder shorts
Channel: Dr. Tracey Marks
Daily Routine for Bipolar Disorder shorts by Dr. Tracey Marks
Period Depression: The SHOCKING Truth Doctors Don't Want You to Know!
Is Your Depression Actually Bipolar? Unmasking the Nuances & Charting a Path Forward
We understand. You’re here because a shadow has settled over your life, a persistent low that whispers doubts and diminishes joy. Perhaps that shadow is labeled "depression." But what if the complexities of your emotional landscape extend beyond that single diagnosis? What if the culprit isn't solely depression, but rather a more complex, often misunderstood, condition: bipolar disorder? Exploring this possibility, and understanding the potential for misdiagnosis, is crucial for receiving the targeted treatment you deserve. This article aims to provide clarity, compassion, and direction, helping you navigate the often-confusing terrain of mood disorders.
The Mask of Depression: Why Misdiagnosis is Common
Depression, in its various forms, presents a familiar face. Feelings of profound sadness, hopelessness, fatigue, and loss of interest in activities once enjoyed are hallmark symptoms. These are also, however, core components of the depressive phases of bipolar disorder. This overlap creates a significant challenge for clinicians. When a patient presents primarily with depressive symptoms, a diagnosis of major depressive disorder (MDD) is often the initial conclusion. But the story doesn't always end there. The presence of cyclical mood changes, subtle shifts in energy, and a history of hypomanic or manic episodes, even if not immediately apparent, can begin to unravel the true picture. It’s easy to see why many individuals find themselves on a treatment path for depression for years before the possibility of bipolar disorder is even considered. This is not necessarily a failing of the medical establishment; rather, it is a testament to the intricate nature of mood disorders and the nuanced ways in which they manifest.
Beyond the Blues: Unveiling the Spectrum of Bipolar Disorder
Bipolar disorder isn’t a monolith. It exists on a spectrum, with varying degrees of severity and symptom presentation. While the stereotypical image might conjure up images of extreme mania and crippling depression, the reality is often far more subtle and individualized. It’s vital to understand the different types:
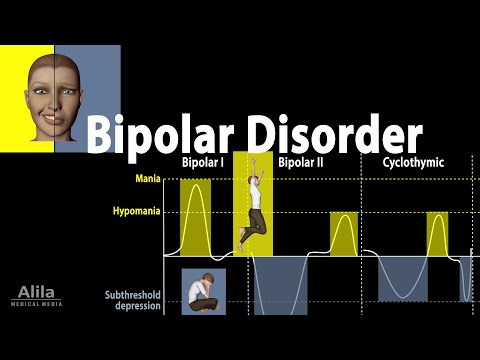
- Bipolar I Disorder: Characterized by the presence of at least one manic episode (a period of elevated mood, increased energy, and often impulsive behavior) that may be preceded or followed by hypomanic or major depressive episodes. Manic episodes are often severe enough to require hospitalization.
- Bipolar II Disorder: Defined by major depressive episodes and hypomanic episodes. Hypomania, unlike mania, is a less severe form of elevated mood and energy. While a person experiencing hypomania may feel highly productive, creative, and energized, their social or occupational functioning is generally not severely impaired.
- Cyclothymic Disorder: A chronic mood disorder characterized by numerous periods of hypomanic symptoms and depressive symptoms that do not meet the full criteria for a major depressive episode. These mood swings fluctuate over a two-year period in adults (one year in children and adolescents).
- Bipolar Disorder, Other Specified and Unspecified: Diagnoses that do not meet the full criteria for the above subtypes, but still display bipolar features.
The Hypomanic "Highs": Recognizing the Subtle Signals
One of the most challenging aspects of bipolar disorder is recognizing the "hypomanic highs." These periods are often experienced as positive – a burst of creativity, increased energy, and a feeling of invincibility. However, these elevated moods can lead to risky behaviors, poor decision-making, and ultimately, a crash into depression. Key indicators of hypomania to watch out for include:
- Elevated Mood: A feeling of being unusually cheerful, optimistic, or irritable.
- Increased Energy: Feeling restless, needing less sleep, and having a seemingly boundless supply of energy.
- Racing Thoughts: Rapid speech, difficulty concentrating, and a feeling that your thoughts are racing.
- Impulsivity: Engaging in activities that are out of character, such as excessive spending, reckless driving, or impulsive decision-making.
- Increased Creativity: Heightened artistic talent and innovative ideas.
- Inflated Self-Esteem: Exaggerated belief in one's abilities and importance.
The problem is these are often associated with positive changes and can be challenging for people to identify these episodes as anything other than a period of increased productivity.
The Downward Spiral: The Devastating Impact of Untreated Bipolar Disorder
The consequences of not addressing bipolar disorder can be devastating. The untreated cycles of depression and mania (or hypomania) can wreak havoc on every facet of life. Relationships suffer, careers are jeopardized, and the risk of substance abuse, self-harm, and suicidal ideation increases significantly. The severity of the disorder can also fluctuate over time. Without proper treatment, the depressive episodes may become more profound and more frequent, while manic episodes may become more dangerous and destructive.
Seeking Answers: The Crucial Steps to Accurate Diagnosis
If you suspect that your depression might be something more, or if your current treatment isn't providing adequate relief, taking the following steps is crucial:
- Comprehensive Evaluation: Seek a thorough evaluation from a qualified mental health professional, such as a psychiatrist or a psychologist. This evaluation should involve a detailed discussion of your symptoms, including their duration, frequency, and severity. The professional should also discuss your family history of mood disorders, any past history of substance abuse, and any previous treatments you've tried. In particular, you should be prepared to discuss any patterns of mood elevation (hypomania or mania) you’ve experienced, even if you initially perceived them as positive or productive. Sharing detailed information is the foundation of diagnosis.
- Keep a Mood Journal: Tracking your mood, sleep patterns, energy levels, and any other relevant symptoms can provide invaluable insights. A mood journal will help you gain a better understanding of your mood fluctuations and share that information with your doctor. This journal also helps you determine if you have ever experienced periods of mania or hypomania.
- Honest Self-Reflection: Be honest with yourself and your healthcare provider. Don't minimize your symptoms, even if they seem embarrassing or difficult to discuss. The more open and forthcoming you are, the more accurate the diagnosis is likely to be.
- Consider a Second Opinion: If you're unsure about the diagnosis you've received, don't hesitate to seek a second opinion from another qualified mental health professional.
- Educate Yourself: Understand the different types of mood disorders, the symptoms, current treatment options and the importance of compliance. The more you know, the better equipped you will be to advocate for yourself and manage your condition effectively.
Treatment Strategies: Charting a Course to Stability
Once a diagnosis of bipolar disorder is confirmed, a comprehensive treatment plan is essential. Treatment typically involves:
- Medication: Mood stabilizers (such as lithium, valproate, and lamotrigine) are the cornerstone of treatment. Antidepressants can be used cautiously in some cases, but they can sometimes trigger manic episodes and should only be used under close medical supervision. Antipsychotic medications are sometimes used to control acute manic episodes.
- Psychotherapy: Cognitive Behavioral Therapy (CBT) and other types of therapy can help you manage your symptoms, develop coping skills, and improve your overall quality of life. Therapy can also help you identify and manage triggers for mood episodes.
- Lifestyle Modifications: Regular sleep, a healthy diet, and regular exercise are essential for managing bipolar disorder. Avoiding triggers, such as stress and substance abuse, is also crucial.
- Support Groups: Connecting with others who understand the experience of living with bipolar disorder can provide invaluable support and a sense of community. Support groups help you learn strategies for managing the condition.
The Path Forward: Hope and Healing Are Possible
Being diagnosed with bipolar disorder can feel overwhelming. However, with the right treatment and support, anyone managing this condition can live a full, productive, and meaningful life. By understanding the complexities of mood disorders, actively participating in your treatment, and embracing self-care strategies, you can gain control over your symptoms and chart a course toward stability and well-being. Remember, you are not alone. There is help available, and recovery is possible. Don't give up on yourself; embrace the journey towards healing and a brighter future.

