
Title: BiPolar Disorder or Depression
Channel: MedCircle
BiPolar Disorder or Depression by MedCircle
can bipolar disorder cause depression, does bipolar disorder cause depression, can bipolar disorder lead to depression, can you have bipolar disorder and depression, can someone have bipolar disorder and depression, can postpartum depression cause bipolar disorder, is depression linked to bipolar disorder, can anxiety and depression lead to bipolar disorder, can depression lead to bipolar, does bipolar cause depression
Is Bipolar Disorder Secretly Hiding YOUR Depression?
Is Bipolar Disorder the Silent Shadow Behind Your Depression?
Have you ever felt like your mood swings are on a wild roller coaster? Depression might seem like the only issue. But, is there something more subtly at play? Sometimes, the answer might be a curveball: bipolar disorder. It can masquerade as something simpler.
Unmasking the Complexity: Beyond the Gloom
Depression is a well-known adversary. However, it's not always the whole story. Bipolar disorder goes beyond simply feeling down. It involves a spectrum of moods. You might experience periods of deep despair. Then, you could shift into manic highs. These highs can be euphoric. They can also be incredibly disruptive.
Furthermore, the lines between these states can blur. Because of that, a diagnosis can be challenging. It is especially true if only the depressive episodes are evident. Think of it like this: depression is the stage. Bipolar disorder is the entire play. It includes the highs and the lows.
The Elusive Link: When Two Worlds Collide
Often, people seek help for their depressive symptoms. They may feel hopeless. They may struggle with sleep or appetite. The diagnosis could be straightforward. Treatment, however, might not yield the expected results. Why? Because, secretly, bipolar disorder might be the root cause.
Consider this: traditional antidepressants can sometimes trigger mania. That's why careful assessment is essential. The best approach involves looking at a comprehensive picture. It is more than just the current mood. Assess the past patterns of behavior. Explore any family history of mental illness also.
Spotting the Silent Clues: Unveiling the Hidden Symptoms
How can you tell if it's more than just depression? Keep an eye out for some key indicators. Have you experienced periods of elevated mood? Have you felt unusually energetic or talkative? Do you struggle with impulsivity or risky behaviors? These are subtle clues. They may suggest the presence of bipolar disorder.
Also, look for changes in sleep patterns. Have you found yourself needing less sleep than usual? Maybe your thoughts race, preventing you from resting. These differences are big red flags. Another aspect to consider is a significant change in your social habits. Are you more outgoing? Are you more irritable? These could also be signs.
Navigating the Path Forward: Seeking Clarity and Support
So, what if you suspect bipolar disorder? Start by talking to mental health professionals. A psychiatrist or psychologist can provide thorough assessments. They can explore your complete history. They can use validated diagnostic tools.
Next, be honest and open about your symptoms. Share any highs, lows, or unusual behaviors. These details will help with an accurate diagnosis. Understand that it might take some time. Finding the right treatment can be a process. Don't get discouraged.
Tailoring the Treatment: Finding the Right Strategy
Treatment for bipolar disorder typically involves a combination of approaches. Medication is often a first step. Mood stabilizers are essential. They help to regulate the extreme mood swings. Antidepressants may be prescribed. However, they are used very cautiously.
Moreover, therapy plays a crucial role. Cognitive behavioral therapy (CBT) is often very effective. It teaches you to manage your thoughts and behaviors. Other types of therapy can provide support. It can teach coping strategies. It can also help you understand your illness.
Living Well with Bipolar Disorder: A Path to Well-being
Living with bipolar disorder is possible. It definitely requires proactive management. Learn more about the condition. Educate yourself about your own triggers. Develop coping mechanisms. Focus on self-care. That includes regular exercise. Sleep hygiene is also important.
Also, prioritize a healthy lifestyle. Limit alcohol and drug use. Join a support group. Connecting with others who understand can be incredibly helpful. Always remember that you are not alone. This can be challenging, but living a fulfilling life is possible.
The Takeaway: Embracing Awareness and Seeking Help
Is bipolar disorder hiding behind your depression? It’s a valid question to ask. It is essential to be aware of the possibilities. If you suspect something more is going on, see a professional. Proper diagnosis and treatment are possible. You can reclaim your life. You can manage your mental health. Don't hesitate to seek help. Because you deserve to feel better.
Is This Silent Killer Stealing Your Joy? (Free Bipolar Depression Test)Here's the article:
Is Bipolar Disorder Secretly Hiding YOUR Depression?
Ever felt like you're riding an emotional rollercoaster, one day soaring high and the next plummeting into the depths of despair? We understand. The world of mental health can be a confusing labyrinth, and often, what seems like straightforward depression might have a secret, more complex identity: bipolar disorder. We're not here to diagnose, because that's a job for the professionals, but we are here to explore the intriguing question - could bipolar disorder be masquerading as your depression?
1. The Mask of Melancholy: Why Depression Can Deceive
Depression, that heavy cloak of sadness and hopelessness, is a familiar foe for many. It can manifest in various ways, from persistent low moods and loss of interest to changes in sleep, appetite, and energy levels. But here's the twist: sometimes, behind that mask of melancholy, a different beast lurks. This "beast" is bipolar disorder, characterized by dramatic shifts in mood, energy, and activity levels. These shifts are what distinguish bipolar disorder from regular depression.
Think of it like this: depression is a deep, dark ocean, and bipolar disorder is a tempestuous sea. Both can feel overwhelmingly difficult to navigate, but the currents, the tides, and the undertow are different. The challenge? Sometimes, only the "dark ocean" (depression) seems visible.
2. Decoding the Symptoms: Depression vs. Bipolar Depression
The key to unraveling this mystery lies in recognizing the nuances of the symptoms. While both conditions share common ground (low mood, fatigue, difficulty concentrating), crucial differences exist.
- Depression: Typically, depression presents as a consistent, prolonged period of low mood, with feelings of sadness, hopelessness, and a loss of interest in activities.
- Bipolar Depression: This presents with similar symptoms, but, it's crucial to realize that it exists within the context of mood swings. This "up" stage, known as mania or hypomania, is the missing piece of the puzzle.
3. Unmasking Mania: The Elusive "Up" Cycle
Here's where things get interesting. The hallmark of bipolar disorder isn't just depression; it's the presence of manic or hypomanic episodes. Mania is a distinct period of elevated mood, energy, and activity. Hypomania, its milder cousin, can be easily overlooked.
Consider this scenario: you've been struggling with what you thought was depression, but you've also experienced periods of increased energy, racing thoughts, impulsivity (spending sprees, risky behaviors), and a reduced need for sleep. These highs, though often short-lived or less readily apparent, are the critical clues hinting at bipolar disorder.
4. The Spectrum of Bipolar: Beyond the Black and White
Bipolar disorder isn't a monolithic condition. It presents itself as a spectrum. There are different types, each with its unique characteristics:
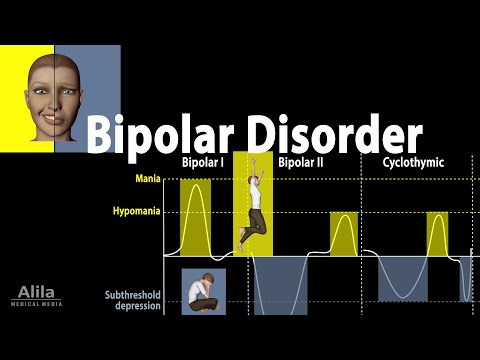
- Bipolar I Disorder: The most severe form, characterized by manic episodes that can last for at least a week and often require hospitalization. It will include a history of major depressive episodes.
- Bipolar II Disorder: Involves major depressive episodes and hypomanic episodes (less severe than mania), but not full-blown manic episodes.
- Cyclothymic Disorder: A milder form involving chronic mood swings, with periods of hypomanic symptoms and depressive episodes that don't meet the full criteria.
Knowing the type is vital for any diagnosis and treatment plan.
5. The Importance of Accurate Diagnosis: A Lighthouse in the Storm
Why is it so important to differentiate between depression and bipolar disorder? Because the treatments and management strategies differ significantly. A misdiagnosis can lead to ineffective treatment and prolonged suffering. Antidepressants, commonly prescribed for depression, can sometimes trigger manic episodes in individuals with undiagnosed bipolar disorder, exacerbating the condition. However, mood stabilizers, and in some cases, other medications, are used to manage bipolar disorder effectively.
Think of it. If you think your house is on fire, your natural urge is to throw some water on it. However, if it's an electrical fire, that wouldn't be the right course of action.
6. Family History: A Glimpses into Your Genes
Genetics play a role in the likelihood of developing bipolar disorder. If you have a family history of the condition, your risk is higher. While genes don't guarantee you’ll develop it, they certainly increase the odds. This is always a piece that we're watching, both in our own lives and in the lives of our loved ones.
7. The Role of Triggers: What Sets the Cycle in Motion?
Stressful life events, trauma, and even seasonal changes can trigger mood episodes in people with bipolar disorder. These are triggers that can create an underlying vulnerability to the specific circumstances.
8. Untangling the Threads: Seeking Professional Help
If you suspect you might be struggling with bipolar disorder, the most important step is to seek professional help. A qualified mental health professional is trained to accurately diagnose and develop an effective treatment plan. This may involve a psychiatrist, a psychologist, or a licensed therapist.
9. Diagnostic Tools: The Clinician's Arsenal
Mental health professionals use a variety of tools to diagnose bipolar disorder. This generally involves a thorough clinical interview, where your doctor will ask you questions about your mood, symptoms, family history, and lifestyle. Sometimes, they may use questionnaires or mood diaries to track your symptoms over time.
10. Treatment Approaches: A Personalized Strategy
Treatment for bipolar disorder is highly individualized. It typically involves a combination of medication, therapy, and lifestyle adjustments.
- Medication: Mood stabilizers (like lithium or some anticonvulsants) are often a cornerstone of treatment. Antidepressants may be used with caution and often in conjunction with mood stabilizers, if necessary, but not as primary treatments.
- Therapy: Psychotherapy, such as Cognitive Behavioral Therapy (CBT) and interpersonal and social rhythm therapy (IPSRT), can help you understand your triggers, manage your symptoms, and develop coping skills.
- Lifestyle Changes: Regular sleep schedules, a healthy diet, and regular exercise can also help to manage your mood and overall well-being.
11. Coping Strategies: Navigating the Ups and Downs
Living with bipolar disorder requires developing effective coping strategies. These can include:
- Creating a routine: Regular sleep, eating, and exercise schedules can help stabilize moods.
- Identifying triggers: Recognizing what sets off mood episodes can help you to avoid or manage them.
- Building a support system: Connecting with friends, family, or support groups can provide emotional support.
- Practicing self-care: Taking time for activities you enjoy and practicing relaxation techniques can help to manage stress.
12. The Power of Self-Awareness: Knowing Your Unique Pattern
Understanding your own personal patterns is fundamental. Keep a mood diary. Note the times of day you're feeling at your peak, your lowest, and how long it lasts. This detailed attention to your own patterns will assist your health professional.
13. Finding Your Balance: Tips for Long-Term Management
Living well with bipolar disorder requires ongoing commitment and self-care.
- Regular follow-up: Stay connected with your mental health professional and attend all scheduled appointments.
- Medication adherence: Take your medications as prescribed, and never stop or change your dose without consulting your doctor.
- Lifestyle management: Continue practicing healthy habits, like a balanced diet, regular exercise, and sufficient sleep.
14. Debunking the Stigma: Seeking Understanding and Support
Sadly, there can be a stigma associated with mental health conditions. It's crucial to remember that seeking help is a sign of strength, not weakness. Talk openly about your experiences, and find a support system that understands and accepts you.
We all have moments of highs and lows in our lives. It's easy to dismiss some of these things. However, you are the most intimate with your own body.
15. A Path Forward: Embracing Hope and Healing
Living with bipolar disorder can be challenging, but it's also possible to live a fulfilling and meaningful life. With the right treatment, support, and self-awareness, you can learn to manage your symptoms, build resilience, and thrive. Remember, you're not alone on this journey. There is hope, and there is healing.
In conclusion, the complex interplay between depression and bipolar disorder can be difficult to decipher. Hopefully, this exploration has shed some light on the potential overlap and highlighted the importance of seeking professional help for an accurate diagnosis and effective treatment. Remember, taking care of your mental health is a journey of self-discovery and continuous growth. Now, if you feel the need to address the question, "Is bipolar disorder secretly hiding your depression?" it's time to consult with a mental health professional.
FAQs
- Can bipolar disorder be misdiagnosed as depression? Yes, that is a distinct possibility, especially in cases where the manic or hypomanic episodes are subtle or overlooked.
- What are the most common signs that suggest bipolar disorder instead of depression? Look for episodes of increased energy, racing thoughts, impulsivity, decreased need for sleep, and a heightened sense of well-being (though this would be a symptom that may be missed).
- How is bipolar disorder treated? Treatment often involves a combination of mood-stabil
Bipolar Disorder Symptoms, Risk Factors, Causes, Diagnosis and Treatments, Animation
By Alila Medical Media Bipolar Disorder Symptoms, Risk Factors, Causes, Diagnosis and Treatments, Animation by Alila Medical Media
Bipolar Disorder vs Depression - 5 Signs You're Likely Bipolar

By Dr. Tracey Marks Bipolar Disorder vs Depression - 5 Signs You're Likely Bipolar by Dr. Tracey Marks

Title: Understanding Bipolar Depression
Channel: Stanford Health Care
Understanding Bipolar Depression by Stanford Health Care
Kidney Stones: Could Your Depression Be to Blame?
Is Bipolar Disorder Secretly Hiding YOUR Depression? Unveiling the Complexities of Mood Disorders
We often find ourselves grappling with the shadows of our minds, those experiences of persistent sadness, hopelessness, and a general disinterest in life that we commonly label as "depression." But what if the experience of this familiar condition is, in reality, masking something far more intricate, a disorder capable of swinging our moods from the depths of despair to the heights of exhilaration: bipolar disorder? The question of whether bipolar disorder is “hiding” depression is complex, and requires us to delve into the nuances of these conditions, exploring their overlapping symptoms and distinct characteristics. It's a journey into the heart of mood regulation, a quest for understanding that unlocks the possibility of more effective treatment and a richer understanding of our own inner worlds.
Deciphering the Depths: Understanding Major Depressive Disorder
Major Depressive Disorder (MDD), the clinical term for what we commonly understand as depression, paints a stark picture. It's a relentless force, characterized by persistent feelings of sadness, emptiness, and a loss of interest or pleasure in nearly all activities. This is, undeniably, a painful reality. Other symptoms often shadow this central core, including significant changes in appetite or weight (either gain or loss), sleep disturbances (insomnia or hypersomnia), fatigue, feelings of worthlessness or excessive guilt, difficulty concentrating, and even thoughts of death or suicide. These experiences can range from mild to severe, significantly impacting a person’s ability to function in daily life. They can affect a person's career, relationships, and overall health.
The diagnostic criteria for MDD, as outlined in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), typically require the presence of five or more of these symptoms during the same two-week period, and at least one of the symptoms must be either depressed mood or loss of interest or pleasure. This framework provides clinicians with a structured approach to identify and diagnose the condition. But the human experience, as we all know, is rarely so straightforward. Many individuals experience depression, and that is the starting point for the many questions leading to where the real problem lies.
The Volatile Spectrum: Exploring the Realm of Bipolar Disorder
Bipolar disorder, on the other hand, introduces a different narrative. It's characterized by significant shifts in mood, energy, activity levels, and the ability to perform daily tasks. The key distinction lies in the cyclical nature of this illness, the oscillation between periods of depression (similar to MDD) and periods of elevated mood, often referred to as mania or hypomania.
During a manic episode, individuals may experience an inflated sense of self-esteem (grandiosity), a decreased need for sleep, increased talkativeness, racing thoughts, distractibility, and impulsive behaviors, such as reckless spending, engaging in risky sexual behavior, or making rash decisions. These actions are not always apparent to the individual, and can have very serious consequences. Hypomania is a less severe form of mania. It still involves elevated mood and energy, but these symptoms are not severe enough to cause significant impairment in daily functioning.
Bipolar disorder exists on a spectrum, with different subtypes categorized based on the severity and frequency of these mood episodes. Bipolar I disorder involves manic episodes that last at least seven days or are so severe that the person needs immediate hospital care. It can also involve depressive episodes. Bipolar II disorder involves depressive episodes and hypomanic episodes, but no full-blown manic episodes. Cyclothymic disorder, a milder form, involves chronic mood swings that don't reach the diagnostic criteria for either mania or major depression, but still represent significant distress and impairment. All of the potential outcomes can severely affect the individual and the closest people in their lives.
The Overlap and the Overlooked: Why Misdiagnosis Occurs
Herein lies the heart of the matter: the potential for misdiagnosis. The symptoms of depression, the very experiences that lead many to seek therapeutic help, are shared across MDD and bipolar disorder. Clinicians, in their attempt to provide proper assistance, must be very careful in the process. A person experiencing a depressive episode, and presenting with symptoms aligned with MDD, might be given a diagnosis and a treatment plan that does not consider the possibility of an underlying bipolar disorder. This is where the problem starts.
The primary challenge stems from the fact that in the absence of a clear history of mania or hypomania, it can be difficult, and sometimes nearly impossible, to differentiate between MDD and bipolar disorder. It's essential to consider the entire picture, including the patient's family history, patterns of mood fluctuations, and responses to previous treatments. When the only symptoms are those of seeming major depression, the process can be slow and complicated.
The consequences of misdiagnosis can be profound. Antidepressant medications, commonly prescribed for MDD, can sometimes trigger or worsen manic episodes in individuals with undiagnosed bipolar disorder. This is the reason that a good doctor will carefully assess the situation. The incorrect approach often leads to a cycle of ineffective treatment and continued suffering. Furthermore, the wrong diagnosis is far more detrimental than the right one.
Unmasking the Truth: Uncovering the Clues within Your Experience
So, how can we begin to discern whether our experience of depression might, in fact, be a mask for bipolar disorder? Awareness, observation, and a willingness to be honest with oneself are the first critical steps.
Consider the following:
- Family History: Does anyone in your family have a history of bipolar disorder or other mood disorders? Genetic predisposition plays a significant role in bipolar disorder.
- Mood Swings: Have you experienced periods of elevated mood, increased energy, or impulsivity that seem out of proportion to the circumstances?
- Response to Antidepressants: Have antidepressants ever made you feel "too good", or triggered mania or hypomania?
- Treatment History: Have previous treatments for depression been unsuccessful, or have you experienced a return of depressive symptoms after initially responding to treatment?
- Cyclical Patterns: Do your moods seem to follow a pattern, with periods of depression alternating with periods of relative stability or elevated mood?
It is extremely important to seek the help of a licensed professional. If a person has any of these symptoms, the need to get help immediately is paramount. A mental health professional, such as a psychiatrist or a psychologist, is best equipped to make an accurate diagnosis. This will involve a thorough evaluation of your history, current symptoms, and family background, as well as a discussion about your treatment options.
Seeking the Right Path: Navigating Treatment and Moving Forward
If you suspect you might have bipolar disorder, the good news is that effective treatments are available. These include a combination of medications (mood stabilizers, antipsychotics, and sometimes antidepressants, carefully monitored and used only when appropriate) and psychotherapy (such as cognitive behavioral therapy (CBT) and interpersonal and social rhythm therapy (IPSRT)).
Mood stabilizers, such as lithium and certain anticonvulsants, are often the cornerstone of treatment for bipolar disorder, helping to stabilize mood and prevent both manic and depressive episodes. Antipsychotics can be used to treat acute manic episodes and to manage psychotic symptoms. The use of antidepressants in bipolar disorder is a more complex issue. All medication should be closely monitored by a physician.
Psychotherapy can provide valuable support and teach coping skills. CBT can help individuals identify and change negative thought patterns and behaviors, while IPSRT focuses on establishing regular daily routines to help stabilize mood.
Beyond the Diagnosis: Embracing a Life of Well-Being
Receiving a diagnosis of bipolar disorder can be challenging, but it is also the beginning of a journey toward understanding and self-discovery. It's not a life sentence of despair, but rather an opportunity to develop strategies for managing your mood, building resilience, and living a fulfilling life.
- Consistency is Key: The more consistent your life is, the better. Routines are essential.
- Education: Learn as much as you can about bipolar disorder. Understanding what your condition is will help you navigate the challenges.
- Support Network: Build a strong support system of family, friends, and a therapist or support group.
- Self-Care: Practice self-care. Prioritize sleep, nutrition, exercise, and stress-reduction techniques.
- Medication Adherence: Take your medications as prescribed and communicate openly with your doctor about any side effects or concerns.
The true healing path begins with recognizing that the question of whether and why our depression might indicate a more complex condition is a path forward. It is a journey of self-discovery, and of personal growth.

